Physical Therapy for Lower Back Pain at Natural Health Center
You will find that most lower back pain is referred to physical therapy as a first-line treatment; guided therapeutic exercises at Natural Health Center strengthen your lower back, condition spinal tissues and joints, and target flexibility and whole-body strength across the kinetic chain. Your short- and long-term goals include restored daily function with less pain; large studies report up to 60% improvement, and your physical therapist will design a tailored program of core, lumbar stabilizing, aerobic, and postural training.
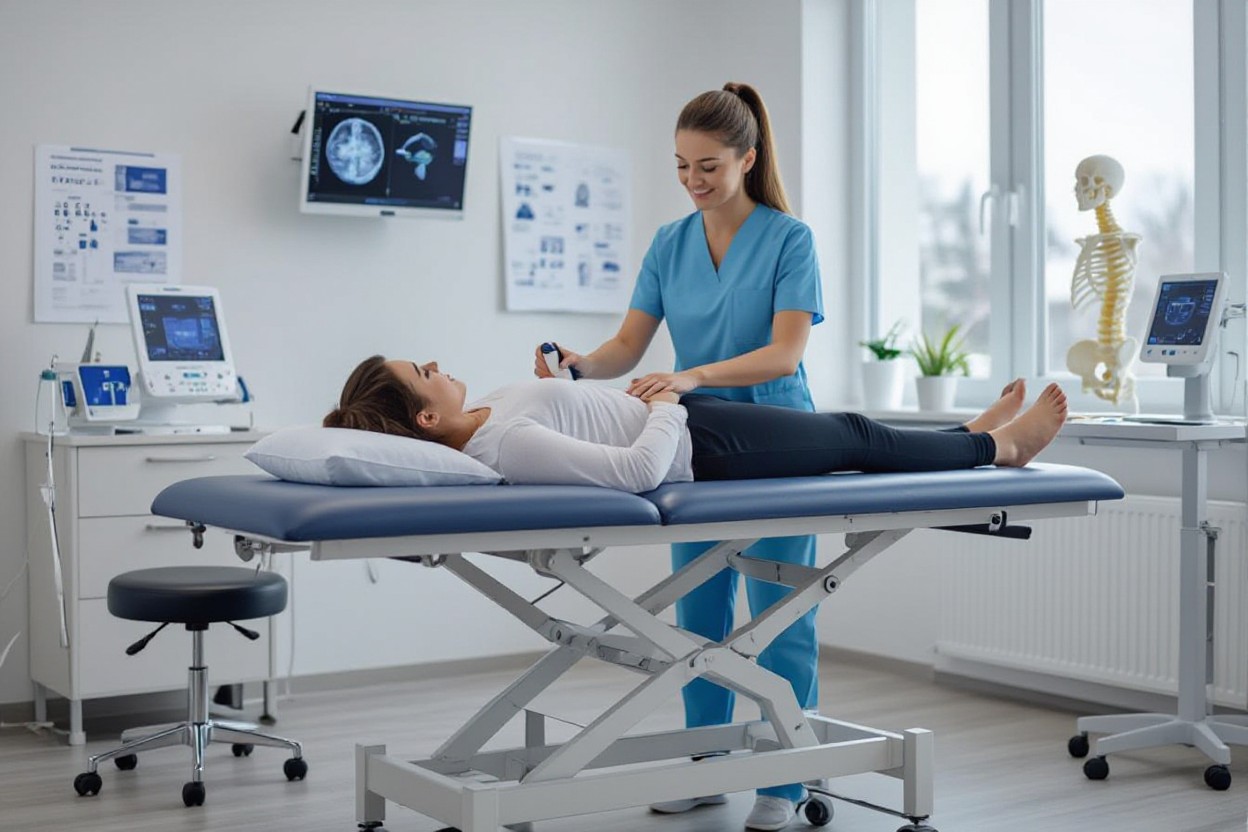
Key Takeaways:
- Physical therapy for lower back pain is a first-line treatment for most lower back pain; Natural Health Center delivers guided therapeutic exercises and education—core-strengthening, lumbar stabilizing, aerobic conditioning, and postural training—to restore function and daily activities, with large studies showing up to 60% improvement.
- Programs are individualized by a physical therapist and teach safe home performance of targeted exercises (pelvic tilts, bird-dog, planks, hamstring stretches, squats, lunges, brisk walking, aquatic therapy) as part of a multi-component plan for strength, flexibility, and endurance.
- Physical therapy benefits axial (nonspecific) back pain, sciatica, and post-surgical recovery; it is not appropriate for emergency conditions (cauda equina, infection, spinal tumors). Duration varies by severity and can be combined with manual therapy, acupuncture, epidural steroid injections, medications, and self-care (heat/cold).
Transforming Pain: The Role of Physical Therapy in Lower Back Recovery
Guided therapeutic programs focus on strengthening your lower back and conditioning spinal tissues and joints across the entire kinetic chain, so muscles, hips, and core share load correctly. You can expect stepwise gains in mobility and function; large-scale studies report up to 60% improvement in pain and related symptoms when programs combine strength, flexibility, posture, and aerobic work.
First-Line Defense against Lower Back Pain
You’ll often be referred to physical therapy as the first-line defense for most lower back pain because therapists teach targeted exercises—core strengthening, lumbar stabilizing, aerobic conditioning, and postural training—that reduce pain, improve movement patterns, and limit recurrence. Typical sessions combine hands-on guidance, progressive home programs, and objective tracking so you can return to daily tasks with less discomfort.
Setting Goals: Short-Term Relief vs. Long-Term Solutions
Short-term goals prioritize pain reduction and restored activity—thinking in weeks—while long-term goals target kinetic-chain strength, flexibility, and prevention over months. You and your therapist will balance symptom relief (reduce flare frequency, sleep better) with functional milestones (sit, lift, walk) and plan progressive loading to move from pain control to durable resilience.
Set measurable benchmarks such as lowering your pain by 2–3 points on a 0–10 scale within 4–6 weeks, improving function by 10–20% on common tools like the Oswestry Disability Index over 8–12 weeks, and regaining specific abilities (sit comfortably for 60 minutes, lift 10–20 lbs, walk 30 minutes). Typical programs involve 1–3 supervised sessions per week plus daily home exercises; adherence, gradual progression, and periodic reassessments guide adjustments toward long-term prevention.
The Anatomy of Recovery: Categories of Therapeutic Exercises
Therapeutic exercises for low back pain are organized into four categories—core strengthening, lumbar stabilization, aerobic conditioning, and postural training—each addressing the kinetic chain so your spine, hips, and legs share load efficiently; large randomized trials report up to 60% improvement in pain and function with guided programs, and your therapist will blend these approaches to restore daily activities with progressive, measurable goals.
Building Core Resilience: Strengthening the Foundation
You build core resilience with targeted moves like pelvic tilts, bird dog, high/low planks, and Swiss ball bridges; begin with 2–3 sets of 8–15 reps or timed planks of 10–20 seconds, progressing by 5–10 seconds as symptoms permit. These exercises increase endurance of the transverse abdominis and multifidus, redistribute spinal loads, and translate directly into easier bending, lifting, and prolonged standing.
Stabilization Strategies: Enhancing Lumbar Support
You develop lumbar stability by activating the hips and deep trunk muscles through hamstring stretches, glute bridges, dead-bug progressions, and single-leg balance work; improving coordination between iliopsoas, gluteus medius, and lumbar extensors reduces aberrant motion and offloads painful segments during everyday tasks like stair climbing and lifting.
Early-phase stabilization emphasizes low-load, high-repetition motor control—transverse abdominis draw-ins, pelvic clocking, and 15–20 rep bridge sets—then advances to resisted bird dogs, side planks, and single-leg Romanian deadlifts as your control and strength improve. Therapists often use real-time feedback (biofeedback, pressure cuff) to retrain timing deficits shown in EMG studies, aiming to normalize recruitment patterns that prevent recurrent instability.
Moving Forward: The Importance of Aerobic Conditioning
You enhance spinal tissue healing and reduce stiffness with aerobic exercise such as brisk walking, stationary cycling, elliptical training, or aquatic sessions; aim for the guideline target of ~150 minutes per week of moderate-intensity activity, which improves circulation, oxygen delivery, and pain modulation in the paraspinal muscles.
Start aerobic work with 10–20 minute sessions and progress to 30–45 minutes, 3–5 times weekly, using low-impact options if you have radicular symptoms. Aquatic exercise allows greater range of motion with less load, and combining aerobic conditioning with strengthening has been shown to produce superior functional outcomes versus either strategy alone.
Posture Matters: The Art of Correct Alignment
You correct posture by establishing a neutral spine during sitting and standing—use a chair with lumbar support, keep feet flat, hips level with or slightly above knees, and set monitor height at eye level; microbreaks every 30–45 minutes and simple pelvic tilts counteract cumulative strain from prolonged sitting.
Implement specific drills like wall angels, thoracic extension over a foam roller, scapular retractions, and seated pelvic tilts to restore thoracic mobility and strengthen postural extensors. Ergonomic tweaks—lumbar roll of ~2–3 cm, 90/90 hip-knee angles, and alternating standing desks for 30–60 minute blocks—reduce forward flexion moments that exacerbate lower back symptoms.
Identifying Pain Points: Conditions That Benefit from Physical Therapy
Most lower back conditions that are not medical emergencies respond to a tailored physical therapy plan: supervised therapeutic exercises improve flexibility, strengthen the kinetic chain, and restore daily function. Studies report up to 60% improvement in symptoms with guided programs combining core work, lumbar stabilization, aerobic conditioning, and postural training, typically delivered over 4–12 weeks depending on severity and goals.
Axial Back Pain: Tackling the Unknown Culprit
Axial (nonspecific) back pain—often present for >3 months—frequently stems from cumulative factors like poor posture, deconditioned core muscles, and excess load on joints; your therapist will prioritize progressive stretching, core- and hip-strengthening, and ergonomic adjustments to reduce pain generators and improve movement efficiency across the spine and pelvis.
Understanding Sciatica: Targeting the Root Causes
Sciatica denotes symptoms from nerve root irritation (e.g., disc herniation, foraminal stenosis, spondylolisthesis) producing leg pain or numbness; you’ll use directional preference exercises (extension/flexion), lumbar stabilization, nerve-gliding techniques, and joint mobilization to unload the nerve and restore mobility, often producing notable relief within 4–8 weeks.
Assessment for sciatica includes neural-tension tests (straight-leg raise), dermatomal sensory mapping, and directional preference screening (McKenzie method) to identify offending movements; a typical plan prescribes clinic sessions 1–3 times weekly plus a daily home program of nerve glides, core work, and progressive aerobic conditioning, with many patients achieving significant pain reduction and functional gains over 6–10 weeks.
Post-Surgical Rehabilitation: Journey Back to Normalcy
After spine surgery you’ll follow a staged rehab plan focused on reducing fatigue, restoring ADLs, and preventing recurrence; early programs emphasize gentle mobility and walking, then advance to abdominal/back/leg strengthening and low-impact aerobic work, with progression guided by surgical type and your surgeon’s clearance.
Typical post-surgical phases span early (0–6 weeks: pain control, gait, light mobility), intermediate (6–12 weeks: progressive strength, balance, 2–3 clinic sessions per week), and advanced (>12 weeks: return-to-work/sport tasks). A structured 6–12 week supervised program plus home exercise often shortens recovery time and improves functional outcomes.
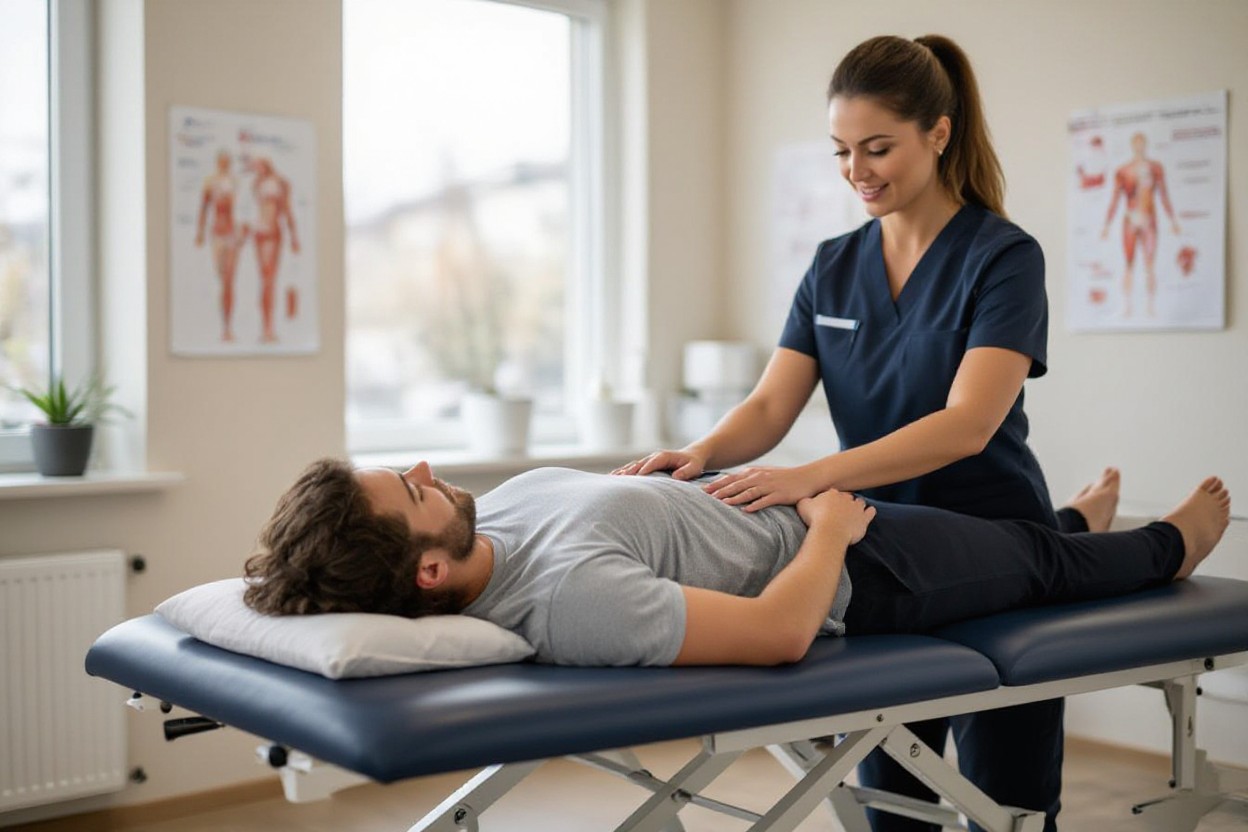
Timeline to Wellness: Understanding the Duration of Physical Therapy
Expect variable timelines: acute low-back flare-ups often improve within 4–6 weeks with 1–2 weekly sessions plus home exercises; subacute cases typically need 6–12 weeks; chronic pain persisting beyond 3 months commonly requires 8–12+ weeks of progressive therapy and lifestyle changes. Large-scale studies report up to 60% symptom reduction when PT is combined with education and targeted exercise, but your individual pace will reflect injury severity, adherence, and medical history.
Personalizing the Journey: Factors Influencing Treatment Length
Several measurable factors shape how long you’ll be in therapy: diagnosis (axial vs radicular), baseline strength and flexibility, pain intensity, surgical history, and work or activity demands. After your therapist tracks objective gains—range of motion, pain scores, functional tests—they’ll adjust frequency, modalities, and the home program to match progress and goals.
- Diagnosis and nerve involvement (e.g., sciatica often needs longer neuropathic-focused care)
- Symptom chronicity: symptoms >3 months usually require extended programs
- Comorbidities: obesity, diabetes, or smoking can slow recovery
- Work demands and ability to modify activities
- Patient adherence to home exercises and activity modification
Integrating Complementary Techniques: Maximizing Outcomes
Combining manual therapy, targeted massage, acupuncture, heat/ice, and, when indicated, epidural steroid injections can accelerate pain relief so you can engage more effectively in strengthening and mobility work; many randomized trials show manual therapy and exercise outperform passive care alone for short-to-midterm gains. Your therapist sequences these modalities to reduce guarding, restore motion, then load the kinetic chain.
Therapists typically begin with pain-control strategies—manual mobilizations, massage to reduce paraspinal spasm, and thermal modalities—then introduce neural mobilization and graded exercise as pain allows. For radicular symptoms, an epidural injection may provide a 2–12 week window of reduced pain that lets you progress rapidly through lumbar stabilization and aerobic conditioning. Practical tactics you’ll use include 15–20 minutes of moist heat before stretching to improve tissue extensibility and 10–15 minutes of ice after acute flares to limit inflammation. Coordination with your physician for injections or medications and tracking functional milestones (e.g., sitting tolerance, walking distance) ensures complementary treatments are time-limited and goal-oriented.
To wrap up
Drawing together, physical therapy for lower back pain gives you a structured program of exercises, education, and hands-on care that restores function, reduces pain by up to 60%, and teaches you techniques to prevent recurrence. Work with a therapist to tailor core, stability, aerobic, and posture training so your daily activities become easier and more comfortable.
Contact us today at Natural Health Center where our collaborative care of physical therapy, chiropractic care, medical massage and more can provide an all under one roof solution to your lower back pain.
FAQ
Q: What is physical therapy for lower back pain and how does it help?
A: Physical therapy for lower back pain is a guided, non-surgical program of education, therapeutic exercise, manual techniques, and self-care aimed at restoring function and reducing pain. Goals include improving flexibility and strength across the kinetic chain (spine, hips, pelvis, legs), conditioning spinal tissues and joints, and returning patients to daily activities with little-to-no discomfort. Large-scale studies report up to about 60% improvement in symptoms with appropriate physical therapy. At Natural Health Center, therapists assess movement, design individualized plans, and teach safe exercise technique so patients can progress independently.
Q: What types of therapeutic exercises are used in physical therapy for low back pain?
A: Therapeutic exercise programs typically combine four categories: 1) Core-strengthening exercises to build abdominal, spinal and pelvic muscle endurance (examples: pelvic tilt, bird dog, high/low planks, Swiss ball work); 2) Lumbar stabilizing and hip/leg exercises to improve support and coordination (examples: hamstring stretches, squats, lunges, planks with leg lifts); 3) Aerobic conditioning to increase circulation and tissue healing (examples: brisk walking, stationary bike, elliptical, aquatic exercise); 4) Postural training to reduce unsupported strain and stabilize the spine (examples: pelvic tilts, seated squats, calf stretches, abdominal strengthening). Natural Health Center combines these approaches to match the underlying cause and patient ability.
Q: Which types of lower back pain are likely to benefit from physical therapy?
A: Most non-emergency lower back conditions can benefit from physical therapy. Common indications include chronic axial (nonspecific) back pain—where PT focuses on stretching, strengthening, and lifestyle modification—sciatica symptoms related to nerve irritation (managed with extension/flexion exercises, lumbar strengthening, nerve/joint mobilization), and post-surgical rehabilitation (progressive core, back and leg strengthening plus aerobic work to restore function). Physical therapy is not recommended as sole treatment for emergencies or serious conditions such as cauda equina syndrome, active spinal infection, or spinal tumors, where immediate medical or surgical care is required. Natural Health Center conducts examinations to determine appropriate candidacy for therapy.
Q: How long does a physical therapy program for lower back pain take and what outcomes can I expect?
A: Program length varies with severity, chronicity, and patient progress; some patients improve in weeks while others require months of guided care. Therapists reassess outcomes and adjust frequency and duration as needed. Expected outcomes include increased flexibility and strength across the kinetic chain, improved daily function, reduced pain, and lower recurrence risk; many patients experience substantial symptom reduction—studies indicate improvements around 60% in many cases. Natural Health Center provides individualized timelines and tracks progress to optimize results.
Q: What happens during physical therapy sessions and what other treatments or self-care are commonly used?
A: Sessions include an initial assessment, hands-on techniques when indicated, supervised exercise instruction, posture and movement retraining, and education on activity modification. Therapists teach correct exercise technique so patients can continue independently and prescribe home-based self-treatments such as heat/cold for pain and inflammation control. PT is often combined with other non-surgical modalities—massage, manual therapy, acupuncture, or, when coordinated with a physician, lumbar epidural steroid injections and analgesic medications—to improve overall outcomes. Natural Health Center offers integrated care plans that combine in-clinic therapy with home programs and coordinated referrals when needed.
